Facts
This contagious disease is caused by a fungal infection, specifically by the dermatophyte fungi.
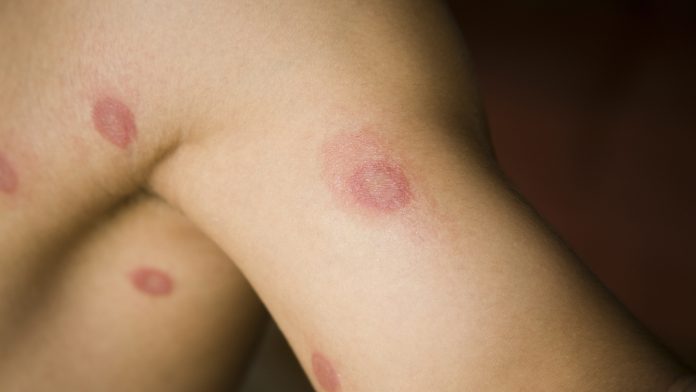
Ringworm was given it’s name because the rash appears worm-like, in round patches on the skin.
Ringworm can occur on the body (especially the stomach or chest area), the scalp or even sometimes, on the nails.
Ringworm is also known as tinea.
Incubation period
Incubation period
The incubation period is the length of time it takes from being infected by someone else with ringworm, to showing symptoms. It will take 4-10 days before you show any symptoms.
Ringworm has an incubation period of: 4-10 days
Catching ringworm
How do you get ringworm?
You can catch ringworm by:
- person to person contact
- contact with animals
- from the soil (if that is where the fungi are present)
Symptoms
Symptoms of ringworm
- On the scalp – this is known as tinea capitis and symptoms are:
- Scaly, round, itchy and bald patches
- Raised inflamed skin
- On the body – this is known as tinea corporis and symptoms are:
- Rashes that are ring-like and may be red, scaly and itchy
- Small blisters around the edge of patches
- The centre of the round patch clears first
- On the nails – this is known as tinea unguium and symptoms are:
- Discolouration of the nails
- Thick or brittle nails
Treatment
Treatment of ringworm
- See a doctor – any child with suspected ringworm needs to see a doctor who can perform an examination to diagnose this condition
- Samples – the doctor may take samples of skin scrapings, hair or nail clippings to be tested in order to identify the infection type
- Medication – the doctor will most likely prescribe some type of anti-fungal medication, either oral (for scalp, nail or body ringworm) or topical (for body ringworm)
- Separate personal care – the child’s brush, comb and towel should be kept separate to everyone else’s in the family, to prevent the infection from spreading
complications
Complications
The complications of ringworm mostly occur due to a weakened immune system. They include:
- hair loss and scarring
- dark marks left on your skin, particularly on darker skin
- nail deformities
- secondary infection if any bacteria entered broken skin
- Majocchi’s granuloma — a rare infection where the fungus has made its way to deeper layers of the skin
Vaccination
Vaccination
There’s currently no vaccine for ringworm.
If your child has ringworm, keep them away from childcare, kindergarten or school. Do not allow them to share any personal items with anyone else.
Risk
Reducing risk of infection
Strategies to reduce infection:
- if your child gets ringworm, keep them away from school and other children
- discuss the ringworm infection with your doctor
- ensure you and your child/children wash hands with a sanitising hand soap
- wash toys and clothes in detergent that has a sanitising effect
- wipe down surfaces with a 70% alcohol solution
- don’t share eating utensils, linens, towels or other personal items with anyone else
References
References
- Ringworm. CDC USA. Accessed 4 July 2024
- Tinea corporis. National Institutes of Health USA. Accessed 4 July 2024
Last reviewed and updated: 4 July 2024