Facts
Pharyngitis is inflammation of the pharynx, the muscular passage at the back of the throat that connects the mouth and nasal cavity to the oesophagus.
The inflammation causes pain, irritation, or scratchiness in the throat, often worse when swallowing.
It can occur on its own or as part of a wider upper respiratory tract infection.
Symptoms
Pharyngitis symptoms
The symptoms of pharyngitis vary from minor to more severe if there is a serious infection:
- Sore, dry, or scratchy throat
- Pain when swallowing
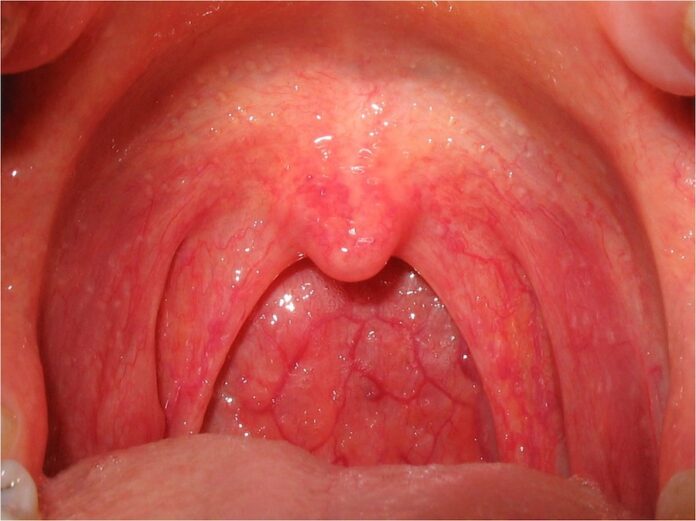
- Red, inflamed pharynx or tonsils
- Swollen lymph nodes in the neck
- Fever or fatigue
- Cough or nasal congestion (viral)
- White spots or pus on tonsils (bacterial)
When to see a doctor
Seek medical attention if you experience any of the following:
- Symptoms last longer than 7 days or worsen
- High fever hiigher than 38.5°C (101°F) or constant cold chills
- Difficulty swallowing, drooling, or breathing
- Rash, joint pain, or swelling (possible strep complications)
- Recurrent sore throats (may indicate reflux, allergy, or chronic infection)/li>
Causes
Causes of pharyngitis
Most cases of pharyngitis are due to a viral infection but some are due to a bacterial infection. And there are non-infectious causes.
Viral infection (about 70%–90% of cases)
- Rhinovirus
- Coronavirus
- Adenovirus
- Influenza and parainfluenza viruses
- Epstein–Barr virus (mononucleosis)
- Coxsackievirus (herpangina, hand-foot-mouth disease)
Bacterial infection (about 5%–30% of cases)
- Group A Streptococcus (GAS) — the main bacterial cause
- Group C or G Streptococcus
- Neisseria gonorrhoeae, Chlamydia pneumoniae, Mycoplasma pneumoniae, Corynebacterium diphtheriae (rare in developed countries)
Non-infectious causes
- Allergies or postnasal drip
- Dry indoor air, smoke or other environmental chemical irritants
- Acid reflux (GERD) causing throat irritation
- Voice overuse or mouth breathing
Prevention
Prevention of pharyngitis
You can’t completely prevent for certain but there are ways you can greatly reduce your risk.
Hygiene prevention factors
- Wash your hands – this is the number one way you can reduce your risk of catching any contagious illness. Always washing your hands thoroughly with soap and water for at least 20 seconds and dry them thoroughly. Wash hands before preparing food. Washing hands after using restrooms. Wash your hands if you have coughed or sneezed into the vicinity of your hands. Wash your hands after blowing your nose into a tissue (or handkerchief)
- Use sanitiser – if you can’t wash your hands, use a sanitiser with at least 70% alcohol content on your hands. This is almost as good as washing your hands with soap and water. Use it at any time you are out of the house and handling anything
- Avoid sharing – do not share any of your personal items (utensils, food, drinks, makeup) with anyone
- Practice cough etiquette – cover your mouth and nose with a tissue when you cough or sneeze. If you don’t have a tissue, cough or sneeze into your elbow or arm. Don’t use your hands
- Stay home when sick – covid-19 taught everyone to stay home when they are sick to prevent making other people sick. Wait until you no longer have any symptoms to go out again. While some workplaces are not as sympathetic to others, you can still wear a mask if you have to be at work and are still not 100% well
- Avoid sick people – minimise contact with anyone who is unwell. If you have to be around unwell people, wear a mask to limit your risk of breathing in airborne germs
Environmental / lifestyle prevention factors
- Quite smoking – don’t smoke and avoid exposure to second hand smoke. Tobacco is a massive throat irritant
- Manage allergies – reducing your allergies will reduce the likelihood you have throat irritation from coughing and sneezing
- Limit chemical irritants – reduce your exposure to environmental chemicals, such as pollution, paint, household cleaners with strong odours and other chemicals as they can irritate the throat
- Avoid touching your face – when you are outside of your home and handling anything, don’t then touch your face, especially your nose, mouth or eyes. This helps prevent germ transmission if whatever you touched was previously touched by a sick person
Complications
Complications of pharyngitis
There are a number of complications of pharyngitis, from the common ones to rare and serious ones.
Common complications
While these complications are common, they won’t happen to everyone.
- Ear and sinus infection – a sore throat can sometimes spread the infection to the ears (otitis media) or the sinuses (sinusitis)
- Abscess – a sore throat can sometimes cause pus to form around the tonsils (peritonsillar abscess) or in other areas of the throat
- Swollen lymph nodes – a sore throat can sometimes cause the lymph nodes in the neck and under the jaw to become swollen and tender
Rare and serious complications
These rare complications which can occur in people with lowered immune systems, the very young or very old. Being very old or very young or having a compromised immune system doesn’t automatically mean you will experience these complications but be aware of them.
- Rheumatic fever – this is a very rare condition in developed countries and mostly occurs in children aged 5-14 years. It can adversely affect the heart, brain, joints and skin. It mostly occurs due to untreated strep throat and scarlet fever infections. In developed countries it’s rare as antibiotics are used to treat strep throat (caused by a bacterial infection). In Australia, the highest incidence is for First Nations people. In developing countries like Africa, it’s mostly due to socioeconomic and environmental facts (overcrowding, limited access to health care)
- Kidney inflammation – post-streptococcal glomerulonephritis is an inflammatory disease which can occur after a strep throat (streptococcal) bacterial infection
- Epiglottitis – this is when the epiglottis, the flap that protects your larynx and allows air into your windpipe and lungs, can get blocked and then it blocks the airways and breathing is not possible. This is life threatening and needs immediately medical attention in hospital
- Mastoiditis – this occurs when the mastoid bone behind the ear, which serves as a protector of the inner ear, gets infected
- Meningitis – a very serious inflammation of the membranes around the brain and spinal cord. Viral meningitis is generally mild, bacterial meningitis is a life threatening medical emergency and needs immediate treatment with antibiotics
Diagnosis
Diagnosis of pharyngitis
A doctor diagnoses pharyngitis through the following:
Physical examination
In the physical examination, the doctor will usually:
- Ask you about your symptoms duration and whether you are also experiencing pain when swallowing, fever, headaches, sore throat, cough, congestion
- Use a thermometer to measure your body temperature
- Use a wooden spatula to depress your tongue so they can look at the back of the throat more closely for redness, swelling or white patches
- Feel your neck for swollen lymph glands
- Check your lungs if you have a cough
Most medical clinics now request you wear a mask if you have upper respiratory symptoms as it could be a coronavirus infection. You may be asked to have a Rapid Antigen Test (RAT) to determine if you have covid-19.
Diagnostic tests
Your doctor may do these test within the clinic or may request you do these at a pathology clinic:
- Rapid antigen detection test – this is a swab of the back of the throat to detect Group A Streptococcus if that bacteria is suspected as the cause of the pharyngitis
- Throat culture – if there is a negative result on the RADT but strep is suspected, the doctor may take a swab of the back of your throat and send it to a pathology lab for testing
- Other lab tests – your doctor may request you have certain blood tests
You should seek medical attention if:
- Your symptoms last longer than 7 days or worsen
- There is a high fever greater than 38.5°C (101.3°F) or continuous cold chills
- Swallowing or breathing feels difficult
- Children or babies are continuously drooling
- There’s a rash, joint pain or swelling (this is a possible strep complications)
<li”>Recurrent sore throats occur as this may indicate reflux, allergy or chronic infection which need to be investigated
Treatment
Conventional treatment of pharyngitis
The conventional, medical treatment is based on whether the pharyngitis is due to a viral or bacterial cause.
Viral pharyngitis
- Usually resolves in 5–7 days.
- Focus is on symptom relief with rest, fluids and pain management.
- Paracetamol or ibuprofen helps pain and fever.
- Antibiotics are not effective and should be avoided.
Bacterial (streptococcal) pharyngitis
- Confirmed with rapid antigen test or throat culture.
- Penicillin V or amoxicillin (10 days) are usually the first-line antibiotics prescribed.
- If you’re allergic to penicillin, you’ll be prescribed azithromycin, clarithromycin or cephalexin instead.
- Early treatment prevents rheumatic fever and kidney inflammation.
Non-infectious pharyngitis
- Avoid the irritant
- Use lozenges, honey, gargling, steam inhalation, herbal tea, probiotics, vitamin C, vitamin D, zinc
- Rest
Prognosis
- Viral – usually gets better in 5-7 days
- Bacterial – usually gets better in 1-3 days with antibiotics
- Non-infectious causes – depends on the cause but supportive therapies can reduce symptom intensity and speed up recovery
Alternative
Alternative / complementary treatment of pharyngitis
These approaches can help reduce inflammation, support immunity and soothe the throat, particularly in viral or mild cases.
Herbal remedies
Marshmallow root (Althaea officinalis)
- Contains mucilage – a soothing gel-like substance that coats mucous membranes
- Eases throat pain, dryness and cough by forming a protective film around the throat
Liquorice root (Glycyrrhiza glabra)
- Anti-inflammatory and antiviral compounds – glycyrrhizin, flavonoids
- Reduces pain and inflammation and soothes throat irritation.
- Gargling liquorice tea helps to soothe a sore throat (don’t drink it, spit it out after gargling)
- Its anti-inflammatory properties are similar to aspirin, so it may also reduce the pain of a sore throat
Sage (Salvia officinalis)
- Antimicrobial and anti-inflammatory (rosmarinic acid, flavonoids)
- Helps kill bacteria and reduce swelling
- A double-blind study found sage spray was as effective as chlorhexidine/lidocaine spray for throat pain. This means it acts like a mild anaesthetic to reduce pain and swelling
Echinacea (Echinacea purpurea)
- Stimulates immune cell activity (macrophages, cytokines)
- Meta-analyses show it has a modest benefit in reducing the duration and severity of colds
Thyme and peppermint
- Contain thymol and menthol — natural antiseptics and mild anaesthetics
- Found in several throat lozenges and sprays
- Freshens breath, eases pain, mild antibacterial effect
Nutrition and supplements
Vitamin C
- Vitamin C supports immune cell function and collagen synthesis for tissue repair
- Food sources – citrus, kiwi, capsicum, all berries
- Supplements – studies show 1g – 3g per day for 7 days, divide larger doses equally throughout the day
Zinc
- Zinc may reduce viral replication in the throat
- Lozenges shorten duration if taken early
- Food sources – oysters, beef, pumpkin seeds
- Supplements – 45mg – 60mg a day, for 7 days, divided up equally throughout the day
Vitamin D
- Enhances immune resilience
- Low levels of vitamin D are linked with recurrent respiratory infections
- Food sources – sunlight, eggs, fortified foods, salmon
- Supplements – 400IU to 1200IU per day for a week
Probiotics
- Some Lactobacillus strains may reduce strep infection recurrence by balancing oral microbiota (the bacteria in the mouth to make sure there’s more good bacteria than bad bacteria and not allowing bad bacteria to take hold)
- Food sources – yoghurt, kefir, probiotic supplements
- Supplements – fthe following strains are shown to help reduce sore throats Streptococcus salivarius K12, Streptococcus salivarius M18, Lactobacillus reuteri, Lactobacillus rhamnosus
Raw honey or Manuka honey
- Antimicrobial / antibacterial
- Coats the throat, reduces cough
- Soothes the throat and reduces inflammation and irritation
- Proven effective in children’s cough studies
- Take 1–2 tsp of raw or Manuka honey in warm water or herbal tea (avoid under age 1)
- Food sources – raw, unprocessed honey or Manuka honey. If choosing Manuka honey, buy one with MGO 260+ (UMF 10+) or higher. You can use higher strength of MGO550+ (UMF10+) for more severe symptoms
Aromatherapy and traditional remedies
Try these methods to help soothe symptoms:
- Steam inhalation may ease congestion and soothe tissues (antiseptic and anti-inflammatory actions).
- Warm saltwater gargle (½ tsp salt in a cup of warm water) helps reduce swelling, clear mucus, and neutralise acidity in the throat.
- Warm herbal teas (ginger, chamomile, mint, peppermint, rooibos) keep mucous membranes hydrated and calm inflammation.
Self care
Pharyngitis self care
You can use these self care strategies to help you heal.
Stay hydrated
- Remember to drink room temperature water. Try not to drink really cold water as that may irritate the throat more
- Drink freshly squeezed juice
- Keeps mucous membranes moist, thins secretions, and supports healing. Aim for warm fluids rather than cold.
Rest and sleep
- Make sure you get enough sleep, 7-8 hours at least
- Immune cells regenerate during rest, speeding up recovery
Humidifier
Invest in a good quality humidifier. Using a cool-mist humidifier reduces dryness, especially in air-conditioned rooms.
Avoid irritants
Tobacco smoke (from smoking and second hand smoke), alcohol, spicy foods and acidic drinks all can worsen inflammation.
Use lozenges or honey lemon
Soothe your throat with lozenges or honey-lemon drinks. This stimulates saliva and coats the throat to reduce dryness and pain. Lozenges with zinc and vitamin C will reduce inflammation and help to heal your throat more quickly.
Honey
Eat raw, unprocessed honey or Manuka honey. If choosing Manuka honey, buy one with MGO 260+ (UMF 10+) or higher. You can use higher strength of MGO550+ (UMF10+) for more severe symptoms.
Gentle breathing
Breathe through your nose to warm and humidify air. Mouth breathing worsens throat dryness and pain.
Good hygiene
Wash your hands frequently, avoid sharing your personal items with others and replace your toothbrush after recovery to prevent reinfection.
Warm compress
This can promote local circulation and comfort. Massage your throat gently with olive oil and put a warm thin compress to help with pain and inflammation.
References
References
- Bisno AL et al. Practice guidelines for the diagnosis and management of group A streptococcal pharyngitis. Clin Infect Dis. 2002;35(2):113–125.
- Shulman ST et al. Clinical practice guideline for the diagnosis and management of streptococcal pharyngitis: 2012 update. Clin Infect Dis. 2012;55(10):1279–1282.
- ESCOP Monographs. Althaea officinalis L. (Marshmallow root). European Scientific Cooperative on Phytotherapy, 2003.
- Wagner H, Jurcic K. Immunological studies of Echinacea extracts. Planta Med. 1992;58(2):163–170.
- Altman RD et al. Efficacy and safety of a sage spray in patients with sore throat. Eur J Med Res. 2006;11(8):371–378.
- Kim JY et al. Licorice gargle reduces postoperative sore throat: randomized controlled trial. Am J Med. 2010;123(11):1079–1084.
- Hemilä H. Vitamin C and infections. Nutrients. 2017;9(4):339.
- Science M et al. Honey for acute cough in children. BMJ. 2012;344:d5159.
- Singh M et al. Zinc for the common cold. J Infect Dis. 2017;216(1):110–119.
- Martineau AR et al. Vitamin D supplementation to prevent acute respiratory infections. BMJ. 2017;356:i6583.
- Corthésy B. Role of probiotics in respiratory infections. Benef Microbes. 2019;10(5):441–455.
- Eccles R. Mechanisms of the placebo effect of sweet cough syrups in treatment of cough. J Pharm Pharmacol. 2020;72(10):1293–1301.
- Sore throat fact sheet. Australian Government Department of Health, 2024.
- Ksenia Babina, Dilara Salikhova, Maria Polyakova, Oxana Svitich, Roman Samoylikov, Samya Ahmad El-Abed, Alexandr Zaytsev, Nina Novozhilova. The Effect of Oral Probiotics (Streptococcus Salivarius k12) on the Salivary Level of Secretory Immunoglobulin A, Salivation Rate, and Oral Biofilm: A Pilot Randomized Clinical Trial. Nutrients. 2022 Mar 7;14(5):1124. doi: 10.3390/nu14051124
Last reviewed and updated: 6 November 2025