Facts
What is Crohn’s disease
Crohn’s disease is one type of inflammatory bowel disease (IBD), the other is ulcerative colitis. Crohn’s disease was named after Dr Burrill Crohn, who together with Dr Leon Ginzburg and Dr Gordon Oppenheimer, first identified the disease in 1932.
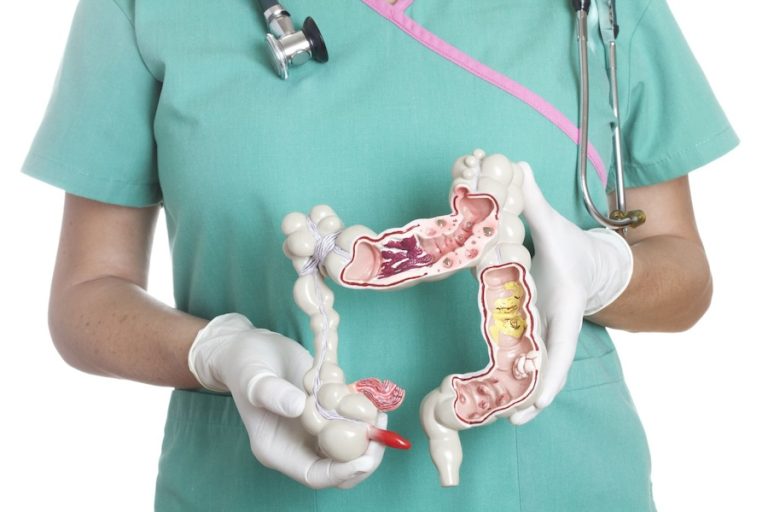
Crohn’s disease can affect any part of the gastrointestinal tract – from the mouth to the anus – but mostly commonly affects the ileum (which is the third part of the small intestine that joins the large intestine (colon or bowel). The colon may also be affected, which can make it difficult to distinguish Crohn’s disease from ulcerative colitis.
Crohn’s disease can affect not just the lining of the bowel, but all the layers of the bowel (from the layers of mucosa to the smooth muscles).
Crohn’s disease is further divided into different sub-conditions depending on which part of the bowel (intestine) is affected:
- Crohn’s colitis – only the large intestine (or colon) is affected
- Ileo colitis – both the small and large intestines (bowel) are affected
- Ileitis – only the small intestine (bowel) is affected
Facts about Crohn’s disease
- People who smoke or more likely to be diagnosed with Crohn’s disease than non-smokers and in fact, giving up smoking can decrease symptoms significantly in some people
- Women who take the contraceptive pill may also have more severe and lengthier episodes of Crohn’s disease than women who do not take the contraceptive pill
- Crohn’s disease is known as an inflammatory bowel disease (IBD)
- Crohn’s disease may cause an malabsorption of vital nutrients and cause weight loss
- Up to 70% of people who have Crohn’s disease need surgery at some point in the course of their disease
- More people have Crohn’s disease than ulcerative colitis (a ratio of 3:2)
- Somewhat more women have Crohn’s disease than ulcerative colitis
- Crohn’s disease causes impaired fat absorption, which means the fat-soluble vitamins (vitamin A, vitamin D, vitamin E and vitamin K) may not be able to be absorbed properly as they need to be absorbed with some fat in order to be able to be digested properly, so this could cause a deficiency in any or all of them
Symptoms
Symptoms of Crohn’s disease
The symptoms of Crohn’s disease depend on how inflamed the gastrointestinal tract is at any given moment.
Crohn’s disease main symptoms
- Abdominal pain – which can be present more often than not, mostly cramping pain (but pain can come and go)
- Anaemia – from malabsorption of iron and/or passing blood in the stools
- Diarrhoea – sometimes with blood and/or mucous
- Fever
- Incontinence – inability to control the flow
- Lethargy and fatigue
- Loss of appetite
- Nausea
- Passing blood in the stools (usually not much and often only detected in a stool test)
- Shooting pain up the backside (tenesmus)
- Vomiting
- Weight loss
Other symptoms
Other symptoms associated with Crohn’s disease are:
- Blurred vision
- Eye problems – inflammation and sensitivity to light
- Headache
- Joint pain
- Mouth ulcers
- Swelling or stiffness of the wrists, elbows, knees, ankles
Crohn’s disease can also make a person more likely to develop gall stones, kidney stones, other kidney and circulatory problems.
Two rare, but serious developments of Crohn’s disease are:
- Liver disease and jaundice (where the skin and other body tissues turn yellow)
- Inability of the blood to clot properly
Causes
Causes of Crohn’s disease
The exact cause of Crohn’s disease is not known. Scientists are yet to find the cause.
Science has put forward a few theories (which are still unproven) about why Crohn’s disease occurs:
- Auto immune disease – Crohn’s disease could be due to the way the immune system responds to certain triggers
- Bacterial or viral infection – some scientists believe that a bacterial or viral infection that occurs in the intestines could trigger Crohn’s disease in some people
- Environment – current research shows Crohn’s disease is not common in people who work outdoors, were breastfed as babies and are from middle-lower socio-economic backgrounds
- Ethnicity – research in the USA shows that people who are Jewish are 2-4 times more likely to get Crohn’s disease than people who are not of Jewish ethnicity
- Food sensitivities – some scientists suggest that Crohn’s disease could be partly due to or triggered by certain food sensitivities which cause a problem in the functioning of the intestines
- Genetics – research shows that about 20% of all people who have Crohn’s disease also have a relative with the condition
Prevention
Prevention of Crohn’s disease
Non-preventable risk factors
Crohn’s disease may be unpreventable in certain circumstances:
- Bacterial or viral gut infection – some medical experts believe that a trigger for Crohn’s disease is a bacterial or viral infection that somehow causes the immune system to function inappropriately. It is believed that this malfunction of the immune system could be one of the reasons why Crohn’s disease is triggered in some people
- Food sensitivity – people with any type of food sensitivity may experience a triggering of worse symptoms, due to the intestines not being able to properly digest and absorb the food, which aggravates inflammation and bloating symptoms
- Genetics – people from certain ethnic backgrounds seem to be more likely to develop Crohn’s disease. There are many reasons hypothesised about this and one of them is the lack of omega-3 fatty acids in their diet and the ratio of omega-3:omega-6 fatty acids being too high in omega-6. This has not been proven, but is one reason that has interesting possibilities because it means that more cases of Crohn’s disease could be preventable based on dietary recommendations
- Lactose intolerance – people who have lactose intolerance can cause Crohn’s disease symptoms to be triggered in the bowel when the lactose is not able to be digested and this causes gas, inflammation and bloating. In addition to this, when symptoms of Crohn’s disease are at their worst, it can cause a temporary (few weeks) lactose intolerance to occur
Preventable risk factors
There may ways to prevent Crohn’s disease symptoms from occurring or reduce worsening of symptoms:
- Antibiotics – some studies show that use of antibiotics (especially long-term) can trigger and make worse the symptoms of Crohn’s disease
- Contraceptive pill – studies show that women who have Crohn’s disease and who also take the contraceptive pill often suffer from more flare-ups of symptoms, than women who do not take the contraceptive pill
- Diet – while diet is not a currently known cause of Crohn’s disease, it is known that following a diet that includes mostly fresh, unprocessed and low fat foods, with plenty of soluble fibre (that has been gradually added to the diet) seems to help symptoms
- Environment – many studies show that Crohn’s disease is not common in people who work outdoors (as they tend to get enough sunlight, exercise and socialising), were breastfed as babies (getting the extra immunity from the mother) and are from middle-lower socio-economic backgrounds (maybe because they tend to eat less meat and more legumes)
- Stress – while not directly causing Crohn’s disease in the first place, stress can aggravate it and make the symptoms worse, so reducing stress is encouraged through some type of relaxation therapy (meditation, tai chi, yoga are all good examples)
Complications
Complications of Crohn’s disease
Crohn’s disease can become complicated and cause a number of further symptoms, some of which can be serious and life threatening:
- Abscess – if any part of the bowel becomes infected and inflamed, it can fill up with pus and cause an abscess to develop, which are treated by antibiotics; sometimes the abscess needs to be drained if the antibiotics do not heal the infection
- Anaemia – many people with Crohn’s disease have deficiency of intrinsic factor, associated with a lack of vitamin B12 (cyanocobalamin) due to malabsorption and this can result in anaemia
- Arthritis – people with any type of inflammatory bowel disease are also at very high risk of also developing arthritis, because this condition is also due to inflammation in the body, so this is yet another complication
- Colon cancer – people with long term, chronic and severe ulcerative colitis may have a higher risk of developing colon cancer, especially because this condition can cause polyp development in the colon, which can become malignant over time
- Dehydration – the person with ulcerative colitis may becomes dehydrated due to the malabsorption problems
- Fistula – this is a small tunnel that links one organ to another which has been formed when an abscess erodes into a neighbouring organ. Fistulas most often occur between the bowel and vagina or the bladder and skin. Surgery is required to remove the fistula and antibiotics are also used to prevent further infection
- Inability of the blood to clot properly – the red blood cells may not be able to clot properly, which means wounds or injuries do not heal properly and this is a high risk factor for internal bleeding. This complication may be due to deficiency of intrinsic factor, associated with a lack of vitamin B12 (cyanocobalamin) due to malabsorption
- Intestinal obstruction – sometimes abscesses can cause scar tissue to be formed when it is healed, which is less flexible than normal tissue in the bowel and may cause a full or partial obstruction of the bowel which means food cannot pass through properly. A full obstruction of the bowel needs urgent surgery to open it up and prevent fatal consequences
- Jaundice – in the condition jaundice, the skin and whites of the eyes turns yellow due to overproduction of the bilirubin, either due to malfunction of the liver or inability of the bile to recycle the bilirubin. The bilirubin is what colours the red blood cells, red
- Liver disease – the liver may stop functioning normally due mainly to other complications of ulcerative colitis, especially malnutrition because of the inability to absorb nutrients from food. Liver disease that can occur as a complication of ulcerative colitis is: cirrhosis, fatty liver, hepatitis
- Malnutrition – people with ulcerative colitis may have malnutrition and deficiency in a number of nutrients, despite eating a healthy diet and this is because of the colon’s malfunction and inability to absorb any nutrients properly or at all. Especially at risk of deficiency are the fat-soluble vitamins and this is because of the colon’s inability to deal properly with fat absorption and these vitamins need some dietary fat in order to be absorbed properly: vitamin A, vitamin D, vitamin E, vitamin K
- Perforation – if the infected abscess bursts, it can cause a rupturing of the colon and pus can leak out
- Peritonitis – if the infected abscess that burst leaks pus into the peritoneum, causing wider-scale infection in the abdominal area. Peritonitis, if not dealt with very quickly can be fatal (surgery is required to get rid of the pus in the peritoneum and remove the part of the colon that is infected)
- Weight loss – people with Crohn’s disease can experience weight loss, due to malabsorption of nutrients from food eaten, due to the colon’s malfunction and inability to absorb nutrients properly or at all
Diagnosis
When to see a doctor about Crohn’s disease
People who have any of the symptoms associated with Crohn’s disease should see a doctor for proper diagnosis to confirm this condition (or to rule it out and confirm another diagnosis).
It is important to see a doctor and not self-medicate, because Crohn’s disease can cause major damage to the intestines and can cause complications if left untreated for a prolonged period.
People with existing Crohn’s disease need to see their doctor (and registered dietician) on a regular basis, to monitor their condition, to ensure they are not suffering from complications and to help with dietary management.
People with existing digestive disorders such as leaky gut syndrome or IBS may also need to see their doctor to rule out Crohn’s disease.
Diagnosis of Crohn’s disease
Initial diagnosis of Crohn’s disease
- Medical history – the doctor will ask a series of questions about your symptoms (especially the duration and severity), your diet, your family medical history (if anyone else has similar symptoms or other gastrointestinal disorders)
- Physical examination – the doctor (or gastroenterologist) will examine your abdominal area for pain or discomfort, as well as examining other parts of your body if needed (your hands, eyes and mouth)
Once the doctor (or gastroenterologist) has reviewed the medical history and determines that further investigation is warranted, the following tests can be ordered:
- Blood test – this is ordered to test iron, haemoglobin, vitamin B12 and other items. A blood test can determine if you are malnourished or have coeliac disease
- Stool sample – this is ordered to determine if there is any blood in the stools or if there is a bacterial infection in the bowel present
Further diagnostic tests
These tests can be ordered if symptoms continue despite treatment:
- Barium meal – is often performed to rule out any other disorders of the bowel, such as ulcers and IBS, as it can show ulcerations of the bowel and stomach, narrowing of the bowel and fistulas in the bowel (little pockets in the bowel). This test is not performed much in Australia any more as a CAT scan can show the same information without having to enduring the ingestion of the barium (less invasive)
- Gynaecological exam – many women with abdominal pain may need to undergo a gynaecological exam to rule out any gynaecological problems, if their symptoms warrant
- CAT scan – a computerised x-ray of the abdominal area which can show if there are any abscesses in any part of the bowel
- MRI – magnetic resonance imaging, can show clear pictures of the body tissues and organs, so it can show abscesses and other abnormalities in the bowel
- Colonoscopy – a gastroenterologist performs this test and it involves having a colonoscope (small, flexible tube with a camera and light at the end) being inserted into the colon (from the anus) to get a better view of the colon (or bowel) and determine level of inflammation and disease progression, and to take a sample of the colon (a biopsy). The colonoscopy is usually performed under light sedation and takes only about 10-15 minutes to be completed
- Video capsule endoscopy – this is a newer test, only recently available, which is used to diagnose Crohn’s disease. A tiny video inside a capsule is swallowed, which gives clear images of the whole gastrointestinal tract as it travels through it. This test is not recommended if there are any suspected bowel obstruction as it can cause a worsening of the obstruction
Treatment
Conventional treatment of coeliac disease
Conventional treatment is based on removing all gluten from the diet and using alternative means of cereals. This usually involves consultation with a dietician who can help to formulate a healthy eating plan without any gluten (no wheat, oats or rye).
The gluten-free diet needs to be followed for life. A registered dietician is the best source for helping to develop a gluten-free diet and assist with implementation.
Gluten-free living requires strict adherence to the special diet and can be difficult at first as it requires a lot of planning, research and guidance.
Some people may have recurrent outbreaks of symptoms and this is usually treated by:
- Corticosteroids – medications such as Prednisone are used to reduce the inflammation in the small intestine if a gluten-free diet is not working well
If coeliac disease is still causing problems (even when following a gluten-free diet and taking the corticosteroids), it could be due to lymphoma (tumour of the white blood cells in the small intestine) and this needs to be treated appropriated (chemotherapy and/or radiotherapy).
Proper diagnosis is required by a medical doctor who can order appropriate tests to determine severity of symptoms and progression of this disease.
Alternative
Alternative / complementary treatment of coeliac disease
Alternative treatment is the same as initial conventional treatment of coeliac disease – following a gluten-free diet for life. It is best to see a qualified naturopath who has studied and specialises in nutrition, or a registered dietician who can develop a treatment plan just for you.
Herbs
There are a few gentle herbs which can be helpful in reducing symptoms associated with this condition:
- Chamomile – an excellent carminative, which helps the digestive system by relieving flatulence, plus it has calming and soothing properties. Chamomile tea is gentle and easy on the digestive system
- Peppermint oil – many studies show that peppermint oil is very effective at reducing spasm in the intestines and so are often prescribed by gastroenterologists for people who have crampy type gastrointestinal pains. Peppermint tea is also useful, but not as effective as the concentrated oil. Some people though, are not able to tolerate the peppermint oil and experience side effect symptoms from trying it – your doctor will advise you if this is suitable for you
- Slippery elm powder – this mucilaginous herb can help to relieve symptoms as it coats the intestinal walls and prevents further damage, pain, symptoms and soothes the intestinal mucosa
Vitamins
Several vitamins are useful in reducing the severity and recurrence of symptoms:
- B vitamins – all of the B vitamins may be especially malabsorbed and this could cause a deficiency which can lead to further adverse health effects
- Folic acid – the B vitamin folic acid may be especially malabsorbed and could contribute to the development of anaemia if a deficiency is serious enough
- Vitamin A – it is very common for people with coeliac disease to be unable to properly absorb fats and therefore fat soluble vitamins such as vitamin A. In addition to this, vitamin A is required to help maintain healthy mucous membranes in the small intestines (but all through the digestive tract) and it also helps the immune system function more effectively
- Vitamin B12 – one of the B vitamins, vitamin B12 may be especially malabsorbed and could contribute to the development of anaemia if a deficiency is serious enough
- Vitamin C – the antioxidant vitamin C is required by the intestines to reduce the damage from this condition and to help the immune system function more effectively in general
- Vitamin D – it is very common for people with coeliac disease to be unable to properly absorb fats and therefore may be deficient in fat soluble vitamins such as vitamin D which require fat for their absorption
- Vitamin E – it is very common for people with coeliac disease to be unable to properly absorb fats and therefore may be deficient in fat soluble vitamins such as vitamin E which require fat for their absorption. In addition to this, vitamin E is a potent antioxidant and deficiency of this vitamin may decrease immune system function
- Vitamin K – it is very common for people with coeliac disease to be unable to properly absorb fats and therefore may be deficient in fat soluble vitamins such as vitamin K which require fat for their absorption
Minerals
Several minerals are useful in reducing the severity and recurrence of symptoms:
- Calcium – the mineral calcium is really necessary to ensure that bone health is maintained properly. People with coeliac disease often have malabsorption of many minerals and it is vital that adequate levels of calcium are absorbed properly to prevent bone loss and ultimately osteoporosis
- Magnesium – the mineral magnesium is necessary to relax the smooth muscles that surround the small and large intestines and enable them to function properly when moving food through. Magnesium is also excellent for enabling the digestive tissue to be less inflamed
- Zinc – the mineral zinc is vital for helping any damaged tissue heal properly and quickly, plus it is vital for the immune system to function effectively and may help to effectively reduce severity and duration of symptoms
Other nutrients
There are several nutrients that are beneficial in reducing severity and recurrence of symptoms:
- Carnitine – in the form acetyl-l-carnitine, helps to heal the stomach and intestines very effectively and quickly (and this effect is enhanced so that it works even better when used in combination with zinc)
- Digestive enzymes – bromelain and other digestive enzymes are excellent at helping the stomach and intestines digest and absorb the nutrients in food properly
- Essential fatty acids – help to reduce inflammation in the body and which can reduce severity and duration of symptoms. The most effective essential fatty acids (EFA) are the omega 3 fatty acids, DHA and EPA and also the omega 6 fatty acid, gamma-linolenic acid (GLA) , which have been shown in many studies to reduce inflammation, especially when taken together in a ratio of 1:1 or 2:1 (ratio of the omega 3:omega 6 fatty acids)
- Glutamine – the conditionally-essential amino acid glutamine is an excellent nutrient for the stomach and small intestine as it helps the intestines function more effectively. In addition, glutamine also helps the white blood cells of the immune system function more effectively too. Glutamine is also needed to make the non-essential amino acid and neurotransmitter GABA, required for mood regulation and relaxation, so this is another way GABA can help to reduce symptoms
- Glutathione – the non-essential amino acid glutathione is an excellent antioxidant for the gastrointestinal tract and especially helps the immune system function more effectively, which helps reduce symptoms
- Probiotics – the live cultures in probiotics help to populate the gastrointestinal tract with “friendly” bacteria that will help with digestion and absorption and reduce some of the symptoms associated with this condition by reducing “bad” bacteria and ensuring proper digestion and absorption of nutrients occurs more effectively
Dietary modifications
There are a number of dietary modifications which should be adhered to help prevent recurrence of symptoms and reduce severity of symptoms:
- Avoid beer and other ales – as they contain gluten or wheat components, which need to be avoided in people following a gluten-free diet
- Drink organic cabbage juice – the juice of cabbage contains “substance U” which has proven ulcer healing properties and it can provide relief for symptoms by healing the mucosa of the intestinal wall, which means it can help reduce (and even prevent) symptoms
- Eat more garlic and onion – these are helpful for improving the function of the immune system in general
- Eat more oily fish – these fish have a higher omega 3 content which provide high dietary levels of the the essential fatty acids which are required to help reduce inflammation in the small intestine. The best fish to eat are: salmon, sardines, trout, mackerel and tuna and the fresher and wilder, the better
- Increase fibre – eat more fresh/raw fruit and vegetables and other non-gluten fibres every day to help the gastrointestinal tract function more effectively by strengthening its functionality. Increase intake of fibre gradually to avoid worsening of symptoms
- Read all food labels – it is vital to read all food nutrition labels to see if there is any gluten in the produce; usually most products will state if it is gluten-free, but if they do not, take care not to use any products with thickeners as they will be gluten based
- Remove all gluten from the diet – all grains (other than millet, corn, chickpeas and brown rice) must be removed from the diet to prevent and reduce symptoms
Lifestyle modifications
There are many changes which can be made to help relieve symptoms of coeliac disease:
- Relaxation – it is really important to help the immune system (and in fact, the whole digestive system too) calm down by engaging in some form of relaxation, such as meditation, tai chi, yoga
Alternative treatments
There are no other alternative treatments recommended for treating coeliac disease.
Always ensure that you notify your medical practitioner of any supplements that you want to take – it may interfere with other medication or conditions you have. Confirm with your doctor it is safe to take before you try it.
Self care
Living with coeliac disease
Coeliac disease requires some diligence in maintaining a specific gluten-free diet, together with some supplementation to help heal the digestive system and reduce severity and duration of symptoms. The following are the strategies most recommended to achieve this:
- Antioxidants – there are a number of antioxidant supplements that are especially recommended for helping reduce symptoms and increase healing capacity (carnitine, glutamine and lipoic acid)
- Avoid cigarette smoke – people who smoke have to give up. This is just another reason to help with the decision to stop smoking. Cigarette smoke causes a number of problems with digestion and should be avoided. People who do not smoke should avoid exposure to second hand smoke from people who smoke around them
- Avoid foods containing gluten – this is probably the most important strategy for avoiding flare-up and worsening of symptoms. If foods are prepared fresh, from scratch, then it is unlikely to find any gluten. When processed foods are purchased, it is very important to read labels as they will have information about the gluten (or not) content in the food. The foods most likely to contain gluten are: wheat, rye, oats, barley, beer, biscuits, crackers, baked goods, some packaged herbs/spices, packaged meals, ice cream, salad dressing, deli meats, chips, packaged soups and sauces
- Dietician – current medical advice recommends that a person who has been diagnosed with coeliac disease should be monitored by a registered dietician who can advise on best foods to eat to prevent worsening of symptoms and help improve quality of life
- Digestive and pancreatic enzymes – the digestive and pancreatic enzymes are released by the digestive to help digest foods that are eaten so that their nutrients can be absorbed through the bloodstream. Digestions starts mainly in the stomach and ends in the small intestine. The digestive and pancreatic enzymes help to increase the amount of food digested by reducing the load on the digestive system and this reduces the amount of undigested foods that may escape into the bloodstream and cause the immune system to respond with an allergic reaction
- Essential fatty acids – the essential fatty acids, especially the omega 3 (DHA/EPA) and omega 6 (GLA) are vital for a properly functioning gastrointestinal system as they reduce inflammation that may be associated with this digestive disorder and this reduces severity and duration of symptoms. The best way to get adequate levels of the essential fatty acids is to eat 3-4 servings of oily fish each week and ensure it is deep ocean, wild fish (not farmed). The fish with the highest levels of omega-3 fatty acids are: mackerel, salmon, sardines, trout, tuna. People who cannot eat fish should try a supplement with balanced levels of each of the essential fatty acids and ensure it has been tested for mercury
- Exercise regularly – physical activity is a must for anyone with a digestive disorder as it helps to increase blood and lymphatic circulation. This helps to eliminate any toxins or unwanted substances more quickly out of the body. Exercise also increases the endorphins released and reduces stress
- Fibre – increasing the amount of fibre in the diet is vital for ensuring healthy digestion. The best types of soluble fibres is psyllium, which helps the intestinal flora digest food properly. The best ways to add psyllium or slippery elm to the diet are in: smoothies, milkshakes, sauces, yoghurt, breakfast cereal, muesli, dips. Suggested dosage is up to 2-3 teaspoons per day, but add it gradually if fibre hasn’t been an integral part of the diet previously, start with 1/2 teaspoon for a few days and add another 1/2 teaspoon every 4 days until at the 2-3 teaspoons a day level
- Gluten free diet – a strict gluten free diet needs to be followed for life (probably) to reduce the allergic reaction to the gluten protein when it is ingested. Many processed foods contain gluten, so nutrition labels need to be read very carefully to ensure that there is no hidden gluten in the food bought. Recent research suggests oats should also be avoided on a gluten-free diet as it causes inflammation to the intestines, which may further exacerbate symptoms. Alternatives to gluten are: rice, corn, millet, quinoa, buckwheat, chickpeas, legumes
- Limit alcohol – it may be necessary to reduce drinking any alcohol while the intestines and the rest of the digestive system are in the process of healing and this is because alcohol is known to irritate the intestines
- Organic – another strategy to reduce the stress on the gastrointestinal system is to avoid foods which are not grown organically (without the use of pesticides and other chemicals and antibiotics). This helps the digestive system because it does not have to also try to detoxify the chemicals in the food in addition to trying to digest foods normally (which is not occurring in this condition). Not only this, but studies show that organic food has higher levels of all their nutrients than food not grown organically
- Probiotics – the “good” bacteria may be in short supply in the digestive system which could be contributing to the symptoms. Acidophilus and other probiotic bacteria are required to help re-populate the intestines with “good” bacteria, which help to properly digest foods and reduce the amount of undigested food that escapes the gut. People who are not lactose intolerant should also include yoghurt that has live cultures
- Reduce stress and relax – prolonged and unrelenting stress is not good for healthy digestion. While stress is not known to cause leaky gut syndrome, it certainly can make symptoms worse because it causes the parasympathetic nervous system to remain in stress mode, which means digestion and absorption is not effective as the nerve that controls it prevents it from happening properly
- Slippery elm – the herb slippery elm is necessary for intestinal health as it is required to heal the intestinal mucosa by providing a mucilaginous layer over the intestinal wall, which reduces the stress on the intestines and helps to heal the intestines more quickly
- Smaller meals – eat smaller meals to help reduce the load on the digestive system, which is not working properly and cannot handle larger meals, which can cause worsening of symptoms when the stomach and intestines struggles to handle the large amount of food eaten. Aim to have around 6 smaller meals each day
- Supplements – certain supplements may be required to help in the healing process by reducing the load on the intestines and reduce symptoms. The fat-soluble vitamins may especially be required because this digestive disorder causes a problem with fat digestion, magnesium to help relax the strong muscles that surround the intestines and also the B vitamins which are needed for healthy nervous tissue and nerve impulses
- Support group – it is advisable to join a support group for people who have coeliac disease, which can provide diet tips, lifestyle tips, information about supplements and a lot of useful information to help improve quality of life
Caring for someone with coeliac disease
Partner
The best way to help a partner with coeliac disease is to be supportive and sympathetic, but also the following can be helpful too:
- Avoiding smoking inside – people with coeliac disease need to be away from any cigarette smoke, as it can exacerbate their symptoms
- Eating smaller meals – help your partner to eat smaller meals by joining them in eating smaller meals, as this helps support your partner a great deal. Cooking and eating smaller meals is one way to help reduce the load on the digestive system by reducing the amount of food that needs to be digested and absorbed
- Encourage a healthy diet – a healthy diet is one which has adequate amounts of fresh fruit and vegetables, wholegrains, legumes, protein and healthy fats and has little or no processed foods
- Encourage exercise – going for walks (or joining a gym together) with your partner is a great way to bond. Exercise helps to improve circulation, reduces stress and encourages better health overall
- Gluten free diet – to help your partner feel less isolated in their often restrictive diet, it may be useful to ensure that all meals prepared in the home are gluten free. This serves two purposes – it gives your partner your support and it also saves time in cooking two different types of meal by just cooking the one
Friends
People who have a friend who has coeliac disease can support their friend by the following:
- Dinner parties – if you invite your friend to a dinner party, try to ensure there is gluten-free food that they can eat. The best way to do this is to ask what foods are off limits for them and ensure to let them know beforehand which foods they should avoid. Gluten is added to many processed foods so always ask
- Discourage alcohol – if your friend has coeliac disease, they should be limiting alcohol intake as it can cause a worsening of symptoms, so try to make your social meetings ones that are alcohol free
Parents
Parents of a child who has coeliac disease can support their child by:
- Avoid smoking inside – people with coeliac disease need to be away from any cigarette smoke, as it can exacerbate their symptoms
- Cooking smaller meals – this is one way to help reduce the load on the child’s digestive system by reducing the amount of food that needs to be digested and absorbed
- Gluten free – ensure all meals cooked for the whole family are gluten free, as this can help your child feel less isolated in their restrictive diet. Always read nutrition labels on foods purchased as there can be gluten hidden in many processed foods
- Probiotics – introduce some probiotics to the child’s diet, preferably in powder form as it can be more easily assimilated into other foods, but the tablets can also be taken if this is not successful
- Psyllium – this soluble fibre is excellent for the whole digestive system as it helps to ensure the correct motion in the intestines, it helps to create proper stools in the colon and it also prevents constipation. Add a little psyllium to smoothies, breakfast cereal, muesli, but ensure it is eaten quickly as it can become gel-like and thick very quickly. Always ensure your child drinks enough water when adding psyllium fibre to their diet
- Slippery elm – find creative ways to add slippery elm to foods (smoothies, breakfast cereal, muesli) in the child’s diet. Slippery elm is one of the herbs most beneficial for any type of digestive disorder, but especially one in which there is irritation and damage to the intestinal wall and the intestinal mucosa
References
References
- Akobeng AK, Richmond K, Miller V, Thomas AG. Effect of exclusive enteral nutritional treatment on plasma antioxidant concentrations in childhood Crohn’s disease. Clin Nutr. 2007 Feb;26(1):51-6
- Belluzzi A, Brignola C, Campieri M, Pera A, Boschi S, Miglioli M. Effect of an enteric-coated fish-oil preparation on relapses in Crohn’s disease. N Engl J Med. 1996 Jun 13;334(24):1557-60
- Brett A, Carson A. Gut Instincts: A Practical Guide to a Healthy Digestive System. 2007, Allen and Unwin, Australia
- Geerling BJ, Badart-Smook A, Stockbrügger RW, Brummer RJ. Comprehensive nutritional status in patients with long-standing Crohn disease currently in remission. Am J Clin Nutr. 1998 May;67(5):919-26
- Kong SC, Hurlstone DP, Pocock CY, Walkington LA, Farquharson NR, Bramble MG, McAlindon ME, Sanders DS. The Incidence of self-prescribed oral complementary and alternative medicine use by patients with gastrointestinal diseases. Clin Gastroenterol. 2005 Feb;39(2):138-41
- Lamb EJ, Wong T, Smith DJ, Simpson DE, Coakley AJ, Moniz C, Muller AF. Metabolic bone disease is present at diagnosis in patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2002 Nov;16(11):1895-902
- Lecleire S, Hassan A, Marion-Letellier R, et al. Combined glutamine and arginine decrease proinflammatory cytokine production by biopsies from Crohn’s patients in association with changes in nuclear factor-kappaB and p38 mitogen-activated protein kinase pathways. J Nutr. 2008 Dec;138(12):2481-6
- Osiecki H. The Physicans Handbook of Clininical Nutrition, 6th Edition. Bioconcepts Publishing QLD, 2001
- Singh B. Psyllium as therapeutic and drug delivery agent. Int J Pharm. 2007 Apr 4;334(1-2):1-14
- Srinivas SR, Prasad PD, Umapathy NS, Ganapathy V, Shekhawat PS. Transport of butyryl-L-carnitine, a potential prodrug, via the carnitine transporter OCTN2 and the amino acid transporter ATB(0,+). Am J Physiol Gastrointest Liver Physiol. 2007 Nov;293(5):G1046-53
- Steinhart AH, Ewe K, Griffiths AM, Modigliani R, Thomsen OO. Corticosteroids for maintenance of remission in Crohn’s disease. Cochrane Database Syst Rev. 2003;(4):CD000301
- Trattler R, Jones A. Better Health Through Natural Healing – How to Get Well Without Drugs or Surgery. 2nd Edition 2001, Hinkler Books, Australia
- Turner D, Zlotkin SH, Shah PS, Griffiths AM. Omega 3 fatty acids (fish oil) for maintenance of remission in Crohn’s disease. Cochrane Database Syst Rev. 2009 Jan 21;(1):CD006320
- Vagianos K, Bector S, McConnell J, Bernstein CN. Nutrition assessment of patients with inflammatory bowel disease. JPEN J Parenter Enteral Nutr. 2007 Jul-Aug;31(4):311-9
- Vicario M, Amat C, Rivero M, Moretó M, Pelegrí C. Dietary glutamine affects mucosal functions in rats with mild DSS-induced colitis. J Nutr. 2007 Aug;137(8):1931-7
- Vilela EG, Torres HO, Ferrari ML, Lima AS, Cunha AS. Gut permeability to lactulose and mannitol differs in treated Crohn’s disease and celiac disease patients and healthy subjects. Braz J Med Biol Res. 2008 Dec;41(12):1105-9
Last reviewed and updated: 14 May 2024