Facts
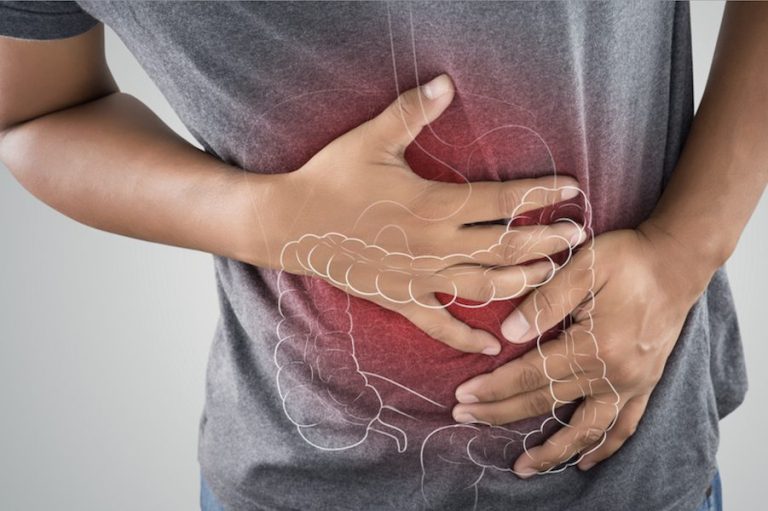
What is inflammatory bowel disease (IBD)
Inflammatory bowel disease (IBD) is a disorder of either the small or large intestines (bowel) and is divided into one of two conditions:
- Crohn’s disease (more prevalent)
- Ulcerative colitis (less prevalent)
The term inflammatory bowel disease is used to cover both the conditions as they have very similar symptoms.
IBD can be serious as it affects not just the bowels, but also other organs and tissues in the body.
IBD is a painful and chronic condition that can severely interfere with digestion and absorption of food, which means that there could be an associated malabsorption of important nutrients (vitamins, minerals, amino acids, fats, carbohydrates, protein) and subsequent malnutrition and unintended weight loss.
For every two cases of ulcerative colitis diagnosed, there are three cases of Crohn’s disease diagnosed.
Since IBD is a chronic health condition, it requires a lot of support to help people deal with the symptoms of this condition.
Facts about IBD
- Inflammatory bowel disease (IBD) is a chronic health condition that usually (but not always) stays with a person for life
- Inflammatory bowel disease (IBD) can cause severe complications if it is not investigated and treated promptly
- There are two types of inflammatory bowel disease (IBD): Crohn’s disease and ulcerative colitis
- There are approximately 45,000 Australians with IBD (around 1 in every 50,000 people), with a similar rate of incidence in New Zealand
- About 120,000 people are diagnosed with IBD in the USA
- Inflammatory bowel disease (IBD) is more prevalent in Western countries and in countries with cooler climates
- Inflammatory bowel disease (IBD) affects men and women at about roughly the same rate of incidence
- Inflammatory bowel disease (IBD) is usually diagnosed in people between the ages of 15-30, but can develop at any age, even in children
- Around 20% of adults with IBD had symptoms from before they were 15 years old
- Inflammatory bowel disease (IBD) is not a contagious disease (even if it was initially triggered by a bacterial or viral infection)
- Inflammatory bowel disease (IBD) is a chronic disorder of the bowel which causes inflammation and pain
- Inflammatory bowel disease (IBD) was first diagnosed in 1934 by Dr Burril Crohn, who described the symptoms as an “inflamed bowel”
Symptoms
Symptoms of inflammatory bowel disease (IBD)
The symptoms of inflammatory bowel disease (IBD) occur mostly in relation to how much and where the bowel is inflamed.
Main symptoms
- Abdominal pain
- Diarrhoea – sometimes with blood and/or mucous, but may not always occur for everyone with IBD
- Fever
- Lethargy and fatigue
- Nausea
- Passing fresh blood in the stools
- Shooting pain up the backside (tenesmus)
- Vomiting
- Weight loss
Other symptoms
Other symptoms associated with inflammatory bowel disease (IBD) are:
- Blurred vision
- Eye problems – inflammation and sensitivity to light
- Headache
- Joint pain
- Mouth ulcers (or canker sores)
- Swelling or stiffness of the wrists, elbows, knees, ankles
- Ulcer-like sores on the skin of the abdomen and legs
Inflammatory bowel disease (IBD) can also make a person more likely to develop gall stones, kidney stones, other kidney and other circulatory problems.
Inflammatory bowel disease (IBD) can also cause serious complications.
Causes
Causes of inflammatory bowel disease (IBD)
The cause of inflammatory bowel disease (IBD) is not known.
Science has put forward a few theories (which are still unproven) about why inflammatory bowel disease (IBD) occurs:
Food sensitivity or allergy
One theory is that inflammatory bowel disease (IBD) could be partly caused by food sensitivity, intolerance or allergy. If there is an existing food sensitivity, but the food continues to be eaten, the bowel is not able to tolerate that food and this causes a whole range of adverse problems in the bowel that prevents proper digestion and absorption of the food through the inability of the “good” bacteria to properly ferment the food and help it to be absorbed, which may cause a proliferation of the “bad” bacteria and worsening of symptoms, inflammation of the bowel and this can then lead to the development of inflammatory bowel disease.
Genetics
Studies show some people of certain ethnicity are more prone to developing inflammatory bowel disease, plus if a family member has it, then it is more likely that it will develop in other family members too.
Immune system problems
Some medical experts believe that inflammatory bowel disease could be due to the way that the immune system responds to certain triggers in the digestive system, in an inappropriate way, that leads to inflammation and the other symptoms associated with inflammatory bowel disease.
Infection
Some medical experts believe that inflammatory bowel disease is initially caused by a bacterial or viral infection in the intestines that continues to inflame the digestive system and ultimately causes symptoms associated with inflammatory bowel disease.
Prevention
Prevention of inflammatory bowel disease (IBD)
Non-preventable risk factors
Inflammatory bowel disease (IBD) may be unpreventable in certain circumstances:
- Bacterial or viral infection – some medical experts believe that a trigger for inflammatory bowel disease is a bacterial or viral infection that somehow causes the immune system to function inappropriately. It is believed that this malfunction of the immune system could be one of the reasons why inflammatory bowel disease is triggered in some people
- Food sensitivity – one theory proposes that inflammatory bowel disorder may be triggered by a food sensitivity that has become worse. The most common types of food sensitivity (or intolerance) are to dairy and gluten
- Jewish ethnicity – studies show that people of Jewish ethnicity have a much higher risk (2-4 times) for developing inflammatory bowel disease than non-Jewish people living in the same geographical area. In addition to this, Jewish people were much more likely to have a relative with this condition (than non-Jewish people)
- Genetics – people from certain ethnic backgrounds seem to be more likely to develop inflammatory bowel disease. There are many reasons hypothesised about this and one of them is the lack of omega-3 fatty acids in their diet and the ratio of omega-3:omega-6 fatty acids being too high in omega-6. This has not been proven, but is one reason that has interesting possibilities because it means that more cases of inflammatory bowel disease could be preventable based on dietary recommendations
- Living in a Western country – there is much less incidence of inflammatory bowel disorder in poorer countries whose diet consists of more legumes, grains and vegetables than in the West, where the diet has more saturated fat (from high meat intake), less fibre and less vegetables
Preventable risk factors
There are ways to prevent IBD from occurring:
- Diet – while diet is not a currently known cause of inflammatory bowel disease, it is known that following a diet that includes mostly fresh, unprocessed and low fat foods, with plenty of soluble fibre (that has been gradually added to the diet) seems to help symptoms
- Environment – many studies show that inflammatory bowel disease is not common in people who work outdoors (as they tend to get enough sunlight, exercise and socialising), were breastfed as babies (get the extra immunity from the mother) and are from middle-lower socio-economic backgrounds (maybe because they tend to eat less meat and more legumes)
- Stress – while not directly causing inflammatory bowel disease in the first place, stress can aggravate it and make the symptoms worse. Reducing stress is encouraged through some type of relaxation therapy. Meditation, tai chi, yoga are all good examples of ways to help destress and relax
Complications
Complications of inflammatory bowel disease (IBD)
There are a number of complications of inflammatory bowel disease (IBD):
- Anaemia – many people with inflammatory bowel disease have deficiency of intrinsic factor, associated with a lack of vitamin B12 (cyanocobalamin) due to malabsorption and this can result in anaemia
- Dehydration – the person with inflammatory bowel disease may become dehydrated due to the malabsorption problems
- Malnutrition – people with inflammatory bowel disease may have malnutrition and deficiency in a number of nutrients, despite eating a healthy diet and this is because of the colon’s malfunction and inability to absorb any nutrients properly or at all. Especially at risk of deficiency are the fat-soluble vitamins and this is because of the colon’s inability to deal properly with fat absorption and these vitamins need some dietary fat in order to be absorbed properly: vitamin A, vitamin D, vitamin E, vitamin K
- Weight loss – people with inflammatory bowel disease can experience weight loss, due to malabsorption of nutrients from food eaten, due to the colon’s malfunction and inability to absorb nutrients properly or at all
Very rare complications
In addition to this, two rare, but serious developments of inflammatory bowel disease (IBD) are:
- Inability of the blood to clot properly – this is a potentially very serious problem which can cause bleeding to occur internally and it is life threatening and an emergency
- Liver disease and jaundice – this is when there is serious disease of the liver, the skin and other body tissues can turn yellow (which can often be the first symptom of a serious liver disease) due to the jaundice. This yellow colouring is due to the colour of red blood cells in the bile
Further serious complications
Inflammatory bowel disease (IBD) can become complicated and cause a number of further symptoms, some of which can be serious and life threatening:
- Abscess – if any part of the bowel becomes infected and inflamed, it can fill up with pus and cause an abscess to develop, which are treated by antibiotics. Sometimes the abscess needs to be drained if the antibiotics do not heal the infection properly
- Perforation – if the infected abscess bursts, it can cause a rupturing of the colon and pus can leak out
- Peritonitis – if the infected abscess that burst leaks pus into the peritoneum, causing wider-scale infection in the abdominal area. Peritonitis, if not dealt with very quickly can be fatal (surgery is required to get rid of the pus in the peritoneum and remove the part of the colon that is infected)
- Fistula – this is a small tunnel that links one organ to another which has been formed when an abscess erodes into a neighbouring organ. Fistulas most often occur between the bowel and vagina or the bladder and skin. Surgery is required to remove the fistula and antibiotics are also used to prevent further infection and reduce symptoms
- Intestinal obstruction – sometimes abscesses can cause scar tissue to be formed when it is healed, which is less flexible than normal tissue in the bowel and may cause a full or partial obstruction of the bowel which means food cannot pass through properly. A full obstruction of the bowel needs urgent surgery to open it up and prevent fatal consequences
- Severe internal bleeding – this can occur during a very severe episode of ulcerative colitis and cause heavy bleeding through the rectum. This condition is life threatening as the patient will need a blood transfusion and possibly surgery to remove the bowel if it does not stop bleeding
- Toxic megacolon – also known as acute dilation. This occurs during a severe episode of ulcerative colitis, which causes the transverse colon to get much bigger than normal and this is life threatening and needs to be treated in hospital with potassium and intravenous fluids or surgery to remove the bowel if it does not improve with treatment
Diagnosis
When to see a doctor about inflammatory bowel disease (IBD)
People who have any of the gastrointestinal symptoms associated with inflammatory bowel disease (IBD) should see their doctor to have a proper diagnosis to confirm whether or not they have this condition. IBD can have serious complications and a medical doctor needs to be consulted.
A doctor is the best person to diagnose this disorder and to rule out any other digestive disorder, which may present with very similar symptoms to inflammatory bowel disease (IBD).
People with existing inflammatory bowel disease (IBD) need to see their doctor if their symptoms change – if the severity of symptoms becomes worse or they experience a different set of symptoms than experienced before.
IBD can have serious complications and a medical doctor needs to be consulted if symptoms get worse.
Diagnosis of inflammatory bowel disease (IBD)
Initial diagnosis of inflammatory bowel disease (IBD) includes:
- Medical history – the doctor will ask a series of questions about your symptoms (especially the duration and severity), your diet, your family medical history (if anyone else has similar symptoms or other gastrointestinal disorders)
- Physical examination – the doctor (or gastroenterologist) will examine your abdominal area for pain or discomfort, as well as examining other parts of your body if needed (your hands, eyes and mouth)
Other tests
If the initial diagnosis warrant it, the following tests can be done to further evaluate the symptoms:
- Blood test – this is ordered to test iron, haemoglobin, vitamin B12 and other nutrients. A blood test can also determine malnourishment or coeliac disease
- Stool sample – this is ordered to determine if there is any blood in the stools or if there is a bacterial infection in the bowel present
Diagnostic tests
Once the doctor (or gastroenterologist) has reviewed the medical history and determines that further investigation is warranted, the following tests can be ordered:
- Barium meal – is often performed to rule out any other disorders of the bowel, such as ulcers and irritable bowel syndrome (IBS), as it can show ulcerations of the bowel and stomach, narrowing of the bowel and fistulas in the bowel (little pockets in the bowel). This test is not performed much in Australia any more as a CAT scan can show the same information without having to enduring the ingestion of the barium (less invasive)
- CAT scan – a computerised x-ray of the abdominal area which can show if there are any abscesses in any part of the bowel
- MRI – magnetic resonance imaging, can show clear pictures of the body tissues and organs, so it can show abscesses and other abnormalities in the bowel
- Colonoscopy – a gastroenterologist performs this test and it involves having a colonoscope (small, flexible tube with a camera and light at the end) being inserted into the colon (from the anus) to get a better view of the colon (or bowel) and determine level of inflammation and disease progression, and to take a sample of the colon (a biopsy). The colonoscopy is usually performed under light sedation and takes only about 10-15 minutes to be completed
- Video capsule endoscopy – this is a newer test, only recently available, which is used to diagnose Crohn’s disease. A tiny video inside a capsule is swallowed, which gives clear images of the whole gastrointestinal tract as it travels through it. This test is not recommended if there are any suspected bowel obstruction as it can cause a worsening of the obstruction
- Gynaecological exam – many women with abdominal pain may need to undergo a gynaecological exam to rule out any gynaecological problems, if their symptoms warrant
Treatment
Conventional treatment of inflammatory bowel disease (IBD)
Mild inflammatory bowel disease
Treatment of mild inflammatory bowel disease (less than four stools per day with no other major gastrointestinal symptoms):
- Topical treatment – a variety of topical treatments can be used to treat symptoms, especially of they occur in the lower end of the colon:
- Enema – a corticosteroid enema is placed in the rectum as a retention enema to help reduce symptoms
- Suppository or foam – a corticosteroid suppository is placed in the rectum as a retention suppository to help reduce symptoms
- Medication – a number of different medications are prescribed depending on symptoms:
- Aminosalicylates – such as sulfasalazine, mesalazine, olsalazine are used for mild to moderate Crohn’s disease and all forms ulcerative colitis
- Antibiotics – are used to treat Crohn’s disease and the complications of Crohn’s disease (fistulas and abscesses), but are generally not used in ulcerative colitis (unless there is an infection or abscess of some sort)
- Glucocorticoids – such as prednisolone, hydrocortisone, budesonide are used to treat Crohn’s disease and ulcerative colitis because their anti-inflammatory properties act very quickly to reduce symptoms. Long-term, these types of drugs can cause a variety of side effects and should never be stopped abruptly as this can cause disruption to hormone levels and cause serious ill health (the dose needs to be tapered gradually to avoid this)
- Vitamin B12 and iron shots – these are given through shots or via a drip as the intestines may not absorb them properly and can cause anaemia through the lack of iron and/or vitamin B12 (a deficiency of either can cause anaemia)
Moderate to severe inflammatory bowel disease
Treatment of moderate to severe inflammatory bowel disease (more than four stools per day with other major gastrointestinal symptoms):
- Immunosuppressants – such as cyclosporine, methotrexate and thiopurine agents are used to treat active Crohn’s disease or ulcerative colitis and to maintain remission in people that have not responded to other drug therapy (glucocorticoids and antibiotics). Thiopurine agents are excellent at helping to heal fistulas. The only downside to these medications is that they can often take months to reach their full effects. The other disadvantage is that using these drugs long term may suppress the immune system too much and raise risk of infection, plus there is also a small risk of lymphoma (cancer of the lymph glands) when using these drugs long term
- Intravenous iron and vitamin B12 – these nutrient are given through shots or a drip as the intestines may not be able to absorb them properly and this can cause anaemia through the lack of iron and/or vitamin B12 (a deficiency of either can cause anaemia)
- Electrolyte and fluid replacement – when inflammatory bowel disease is really severe, replacement fluids including the electrolyte minerals (chloride, sodium, potassium) are given via a drip (usually in hospital) to replace the fluids and electrolytes lost through diarrhoea (and vomiting)
- Total parenteral nutrition – if the inflammatory bowel disease is really severe and absorption of food is greatly impaired because of bowel obstruction, or due to inability to absorb nutrients at all because of the severity of the disease, then total parenteral nutrition must be given via drip in hospital, which allows the gastrointestinal tract to rest and heal. This provides all the nutritional requirements through the blood so that nothing goes through the bowel and this enables the inflammation and other symptoms of the bowel to be healed
Surgery
Surgery is not often recommended as a treatment for Crohn’s disease, because once it is performed, the need for recurrent surgery increases.
The most likely reasons for surgery are for serious complications of this condition such as:
- fistulas
- abscesses
- internal bleeding
- bowel perforation
- cancer
- strictures
- bowel blockages
Alternative
Alternative / complementary treatment of inflammatory bowel disease (IBD)
There are a number of alternative therapies that can be used to treat inflammatory bowel disease, which can help to reduce the severity and length of symptoms. It is best to see a qualified naturopath who can develop a treatment plan just for you.
Never try to self-treat inflammatory bowel disease (IBD), as complications do and can arise.
Herbs
There are a number of excellent herbs which may help to provide relief for symptoms:
- Ginger – the renowned anti-nausea properties of ginger can help reduce symptoms
- Marshmallow – this herb has mucilaginous properties, which means it helps to sooth the mucous membranes and enable quicker healing of the ulcer, reducing symptoms in the process. People with hypoglycaemia or diabetes need to be careful taking this herb as it can reduce blood glucose levels too much when it is taken regularly
- Slippery elm powder – this mucilaginous herb can help to relieve symptoms as it coats the intestinal walls and prevents further damage, pain, symptoms and ulceration
Vitamins
There are a number of vitamins which may help to provide relief for symptoms:
- Vitamin A – the important antioxidant, vitamin A is vitally necessary for healthy mucous membranes in every part of the body and it can also help to speed up healing time. In addition to this, vitamin A is an important antioxidant which helps to reduce the damage to the intestines that inflammation causes and may possibly help reduce the risk of complications by preventing some of the scar tissue from forming. In addition to this, the bowel may not be absorbing the fat-soluble vitamins properly such as vitamin A, due to an inability to absorb fat properly and may be come deficient
- Vitamin B12 – people with inflammatory bowel disease may easily become deficient in vitamin B12 and may require supplementation, as they are not producing enough intrinsic factor to help them absorb it and anaemia could be the result
- Vitamin C – is a potent antioxidant vitamin C, helps to reduce the damage that inflammation causes, plus it helps in the maintenance of healthy collagen
- Vitamin D – people with inflammatory bowel disease may become deficient in the fat-soluble vitamin D because they may not be able to absorb fat properly, which is necessary for the absorption of vitamin D
- Vitamin E – the potent antioxidant vitamin E helps to reduce the damage that inflammation causes, plus it helps to reduce inflammation
- Vitamin K – people with inflammatory bowel disease may become deficient in the fat-soluble vitamin K because they may not be able to absorb fat properly, which is necessary for the absorption of vitamin K
- Multivitamin – a general multivitamin containing all the vitamins is necessary to correct any possible nutrient deficiency, but the most important vitamins are listed above
Minerals
There are a number of minerals which may help to provide relief for symptoms:
- Selenium – the important antioxidant mineral selenium, helps to reduce the oxidative damage that inflammation causes in the body, which helps with the healing process
- Zinc – the other important antioxidant mineral zinc is vital to help the tissues heal more quickly and effectively from any type of damage
- Multivitamin – a general multivitamin containing all of the minerals is necessary to correct any possible nutrient deficiencies, but the most important minerals needed to help with this condition are listed above
Other nutrients
There are a number of other nutrients which may help to provide relief for symptoms:
- Amino acids – all of the 9 essential amino acids should be taken in supplement form to help prevent protein malabsorption. Amino acids are a vital nutrient that the body needs to have from the diet every day
- Antioxidants – are required to reduce the oxidative damage to the digestive tissues that the inflammation this condition causes. Antioxidants also help to ensure the immune system is functioning effectively
- Bromelain – an enzyme (from pineapple) which is especially helpful for proper digestion
- Digestive enzymes – help to maintain proper intestinal digestion and absorption
- Essential fatty acids – especially omega 3 and linoleic acid, which both help to reduce all types of inflammation in the body. The best form to take these is in fish oil, linseed oil, cod liver oil or tuna oil
- Glucosamine – the nutrient glucosamine helps to reduce inflammation in the body in general and also reduces severity of symptoms
- Glycine – the semi-essential amino acid glycine is beneficial in helping reduce the inflammation and thereby also reducing the recovery time from a flare-up of the condition
- Prebiotics – these are the precursors of probiotics, which help to promote the growth of “good” bacteria in the bowel so that they can function properly and keep the bowel healthy. Prebiotics are a type of dietary fibre which cannot be digested by the bowel, so they provide food for the intestinal flora. Examples are: asparagus, garlic, milk, onions, yoghurt
- Probiotics – are living micro-organisms, which are known as “good” bacteria which help the gastrointestinal tract (GIT) fight off any “bad” bacteria, viruses and fungi. Probiotics normally exist in the GIT but can become depleted in people with bowel disease. Probiotics help to maintain a healthier GIT flora and may help reduce symptoms. Try lactobacillus acidophilus
- Quercetin – the super bioflavonoid quercetin helps to reduce inflammation and clotting, which is useful in helping reduce severity and duration of symptoms
- Taurine – the semi-essential amino acid taurine is beneficial in helping reduce the inflammation, which means that it is also useful in reducing the recovery time from a flare-up of the disease
Dietary modifications
There are a number of dietary modification strategies which may help to provide relief for symptoms:
- Avoid refined sugar – as they can cause further intestinal irritation
- Drink organic cabbage juice – the juice of cabbage contains “substance U” which has proven ulcer healing properties and it can help to reduce the ulceration of the bowel (or rectum) mucosa and provide relief for symptoms
- Drink more water – fluids lost need to be replaced and so water is essential to help the bowel function properly, but try to use filtered water as most cities have fluorinated water supplies and the fluoride can irritate the bowel
- Eat foods high in mucopolysaccharides – foods such as tripe, oats, onions, aloe vera, slippery elm help to heal the mucosa (mucous lining) of the intestinal walls and may help to reduce symptoms
- Eat more protein – eat foods high in low fat protein, such as organic chicken and a little low fat red meat, but especially and mainly oily fish (salmon, mackerel, tuna, trout, sardines) which are high in omega 3 fatty acids (which help to reduce inflammation)
- Eat smaller meals – have about 5-6 smaller meals each day to put less stress on the digestive system, which is not functioning as well as it should be. By eating smaller meals, it helps the digestive system because it only has to digest and absorb only a little bit of food at a time
- Limit dairy – some dairy foods (cheese, butter, cream, sour cream, ice cream) can contain carageenan, which is a food additive added as a stabiliser and it may cause intestinal irritation in some people. Always use organic and always check food labels
Lifestyle modifications
There are a number of lifestyle modifications which may help to provide relief for symptoms:
- General relaxation – learn some relaxation therapy such as meditation, tai chi, or yoga to help calm the mind and help calm digestion too. Studies show that stress can have an adverse effect on symptoms, by making them worse
- Rest – people with this condition need to rest properly anyway, but especially during a flare-up as this is when the body needs all its resources to counter the inflammation and heal
- Slow down – take life at a slower pace and relax. Always rushing around can have an adverse impact on digestion in general, but especially so in people with a digestive disorder, as studies show that stress can definitely aggravate symptoms
Alternative treatments
- Food sensitivities – get checked for food sensitivities and/or use an elimination diet to find any food intolerance or food allergies (especially for lactose intolerance or gluten intolerance)
Always ensure that you notify your medical practitioner of any supplements that you want to take – it may interfere with other medication or conditions you have. Confirm with your doctor it is safe to take before you try it.
Self care
Living with inflammatory bowel disease (IBD)
Inflammatory bowel disease (IBD) requires some diligence in maintaining a healthy diet and some supplementation may be required to help heal the digestive system and reduce severity and duration of symptoms.
Self care strategies
The following are the strategies most recommended to achieve this:
- Avoid alcohol – it may be necessary to stop drinking any alcohol while the intestines and the rest of the digestive system are in the process of healing and this is because alcohol is known to irritate the intestines
- Avoid cigarette smoke – people who smoke have to give up. This is just another reason to help with the decision to stop smoking. Cigarette smoke causes a number of problems with digestion and should be avoided. People who do not smoke should avoid exposure to second hand smoke from people who smoke around them
- Digestive and pancreatic enzymes – the digestive and pancreatic enzymes are released by the digestive to help digest foods that are eaten so that their nutrients can be absorbed through the bloodstream. Digestions starts mainly in the stomach and ends in the small intestine. The digestive and pancreatic enzymes help to increase the amount of food digested by reducing the load on the digestive system and this reduces the amount of undigested foods that may escape into the bloodstream and cause the immune system to respond with an allergic reaction
- Essential fatty acids – the essential fatty acids, especially the omega 3 (DHA/EPA) and omega 6 (GLA) are vital for a properly functioning gastrointestinal system as they reduce inflammation that may be associated with this digestive disorder and this reduces severity and duration of symptoms. The best way to get adequate levels of the essential fatty acids is to eat 3-4 servings of oily fish each week and ensure it is deep ocean, wild fish (not farmed). The fish with the highest levels of omega-3 fatty acids are: mackerel, salmon, sardines, trout, tuna. People who cannot eat fish should try a supplement with balanced levels of each of the essential fatty acids and ensure it has been tested for mercury
- Exercise regularly – physical activity is a must for anyone with a digestive disorder as it helps to increase blood and lymphatic circulation. This helps to eliminate any toxins or unwanted substances more quickly out of the body. Exercise also increases the endorphins released and reduces stress
- Fibre – increasing the amount of fibre in the diet is vital for ensuring healthy digestion. The best types of soluble fibres is psyllium, which helps the intestinal flora digest food properly. The best ways to add psyllium or slippery elm to the diet are in: smoothies, milkshakes, sauces, yoghurt, breakfast cereal, muesli, dips. Suggested dosage is up to 2-3 teaspoons per day, but add it gradually if fibre hasn’t been an integral part of the diet previously, start with 1/2 teaspoon for a few days and add another 1/2 teaspoon every 4 days until at the 2-3 teaspoons a day level
- Manage food intolerance or sensitivity – these can be confirmed (if not known) through either an elimination diet or a blood test. An elimination diet involves removal of all the suspected allergens (such as dairy, gluten) as well as all processed foods and associated food additives and then re-introducing these foods, one at a time to determine if they have an adverse effect on digestion, or any other part of the body
- Organic – another strategy to reduce the stress on the gastrointestinal system is to avoid foods which are not grown organically (without the use of pesticides and other chemicals and antibiotics). This helps the digestive system because it does not have to also try to detoxify the chemicals in the food in addition to trying to digest foods normally (which is not occurring in this condition). Not only this, but studies show that organic food has higher levels of all their nutrients than food not grown organically
- Probiotics – the “good” bacteria may be in short supply in the digestive system which could be contributing to the symptoms. Acidophilus and other probiotic bacteria are required to help re-populate the intestines with “good” bacteria, which help to properly digest foods and reduce the amount of undigested food that escapes the gut. People who are not lactose intolerant should also include yoghurt that has live cultures
- Reduce stress and relax – prolonged and unrelenting stress is not good for healthy digestion. While stress is not known to cause leaky gut syndrome, it certainly can make symptoms worse because it causes the parasympathetic nervous system to remain in stress mode, which means digestion and absorption is not effective as the nerve that controls it prevents it from happening properly. Learn some relaxation techniques to help release stress and improve symptoms
- Slippery elm – the herb slippery elm is necessary for intestinal health as it is required to heal the intestinal mucosa by providing a mucilaginous layer over the intestinal wall, which reduces the stress on the intestines and helps to heal the intestines more quickly
- Smaller meals – eat smaller meals to help reduce the load on the digestive system, which is not working properly and cannot handle larger meals, which can cause worsening of symptoms when the stomach and intestines struggles to handle the large amount of food eaten. Aim to have around 6 smaller meals each day
- Supplements – certain supplements may be required to help in the healing process by reducing the load on the intestines and reduce symptoms. The fat-soluble vitamins may especially be required because this digestive disorder causes a problem with fat digestion, as well as a general multivitamin which contains all the vitamins and minerals to prevent malnutrition due to malabsorption and the amino acids (especially taurine and glycine) which help to reduce the inflammation associated with this disorder
Caring for someone with inflammatory bowel disease (IBD)
Partner
The best way to help a partner with inflammatory bowel disorder (IBD) is to be supportive and sympathetic, but also the following can be helpful too:
- Avoiding smoking inside – people with inflammatory bowel disease (IBD) need to be away from any cigarette smoke, as it can exacerbate their symptoms
- Eating smaller meals – help your partner to eat smaller meals by joining them in eating smaller meals, as this helps support your partner a great deal. Cooking and eating smaller meals is one way to help reduce the load on the digestive system by reducing the amount of food that needs to be digested and absorbed
- Encourage a healthy diet – a healthy diet is one which has adequate amounts of fresh fruit and vegetables, whole grains, legumes, protein and healthy fats and has little or no processed foods
- Encourage exercise – going for walks (or joining a gym together) with your partner is a great way to bond. Exercise helps to improve circulation, reduces stress and encourages better health overall
Friends
People who have a friend who has inflammatory bowel disease (IBD) can support their friend by the following:
- Dinner parties – if you invite your friend to a dinner party, try to ensure there is food that they can eat. The best way to do this is to ask what foods are off limits for them and ensure to let them know beforehand which foods they should avoid
- Discourage alcohol – if your friend has IBD, they should be limiting alcohol intake as it can cause a worsening of symptoms, so try to make your social meetings ones that are alcohol free
Parents
Parents of a child who has inflammatory bowel disease (IBD) can support their child by:
- Avoid smoking inside – people with inflammatory bowel disease (IBD) need to be away from any cigarette smoke, as it can exacerbate their symptoms
- Cooking smaller meals – this is one way to help reduce the load on the child’s digestive system by reducing the amount of food that needs to be digested and absorbed
- Fibre – it is important to include some soluble fibre in the child’s diet, slowly and a little at a time (to prevent worsening of symptoms) to help with symptoms. Studies show that a diet high in plant fibre is associated with lower incidence of IBD. Some good sources of fibre are: psyllium (this can be added to cereals and smoothies, but ensure to have adequate amounts of water to enable it to flow through the digestive system properly), vegetables, legumes and cereals
- Probiotics – introduce some probiotics to the child’s diet, preferably in powder form as it can be more easily assimilated into other foods, but the tablets can also be taken if this is not successful
- Slippery elm – find creative ways to add slippery elm to foods (smoothies, breakfast cereal, muesli) in the child’s diet. Slippery elm is one of the herbs most beneficial for any type of digestive disorder, but especially one in which there is irritation and damage to the intestinal wall and the intestinal mucosa
References
References
- Akobeng AK, Richmond K, Miller V, Thomas AG. Effect of exclusive enteral nutritional treatment on plasma antioxidant concentrations in childhood Crohn’s disease. Clin Nutr. 2007 Feb;26(1):51-6
- Arrieta MC, Madsen K, Doyle J, Meddings J. Reducing small intestinal permeability attenuates colitis in the IL10 gene-deficient mouse. Gut. 2009 Jan;58(1):41-8
- Brett A, Carson A. Gut Instincts: A Practical Guide to a Healthy Digestive System. 2007, Allen and Unwin, Australia
- Dubinsky MC, Wang D, Picornell Y, et al. IL-23 receptor (IL-23R) gene protects against pediatric Crohn’s disease. Inflamm Bowel Dis. 2007 May;13(5):511-5
- Geerling BJ, Badart-Smook A, Stockbrügger RW, Brummer RJ. Comprehensive nutritional status in patients with long-standing Crohn disease currently in remission. Am J Clin Nutr. 1998 May;67(5):919-26
- Kong SC, Hurlstone DP, Pocock CY, Walkington LA, Farquharson NR, Bramble MG, McAlindon ME, Sanders DS. The Incidence of self-prescribed oral complementary and alternative medicine use by patients with gastrointestinal diseases. Clin Gastroenterol. 2005 Feb;39(2):138-41
- Lamb EJ, Wong T, Smith DJ, Simpson DE, Coakley AJ, Moniz C, Muller AF. Metabolic bone disease is present at diagnosis in patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2002 Nov;16(11):1895-902
- Lecleire S, Hassan A, Marion-Letellier R, et al. Combined glutamine and arginine decrease proinflammatory cytokine production by biopsies from Crohn’s patients in association with changes in nuclear factor-kappaB and p38 mitogen-activated protein kinase pathways. J Nutr. 2008 Dec;138(12):2481-6
- Lee KM. Nutrition in inflammatory bowel disease. Korean J Gastroenterol. 2008 Jul;52(1):1-8
- Osiecki H. The Physicans Handbook of Clininical Nutrition, 6th Edition. Bioconcepts Publishing QLD, 2001
- Reifen R, Nur T, Ghebermeskel K, Zaiger G, Urizky R, Pines M. Vitamin A deficiency exacerbates inflammation in a rat model of colitis through activation of nuclear factor-kappaB and collagen formation. J Nutr. 2002 Sep;132(9):2743-7
- Singh B. Psyllium as therapeutic and drug delivery agent. Int J Pharm. 2007 Apr 4;334(1-2):1-14
- Tratter R, Jones A. Better Health Through Natural Healing: How to Get Well Without Drugs or Surgery, 2nd Edition. McGraw Hill, 2001
- Vagianos K, Bector S, McConnell J, Bernstein CN. Nutrition assessment of patients with inflammatory bowel disease. JPEN J Parenter Enteral Nutr. 2007 Jul-Aug;31(4):311-9
- Vicario M, Amat C, Rivero M, Moretó M, Pelegrí C. Dietary glutamine affects mucosal functions in rats with mild DSS-induced colitis. J Nutr. 2007 Aug;137(8):1931-7
Last reviewed and updated: 14 May 2024